
How accessible bathrooms can reduce injuries at assisted living facilities
If you asked the average person on the street which professions suffer the most workplace injuries, you’d likely hear such answers as police officers, construction workers and loggers. While it is absolutely true that these jobs can be dangerous, what may be less well known is that direct care workers who assist patients, the elderly and disabled residents also face serious physical risks on a daily basis.
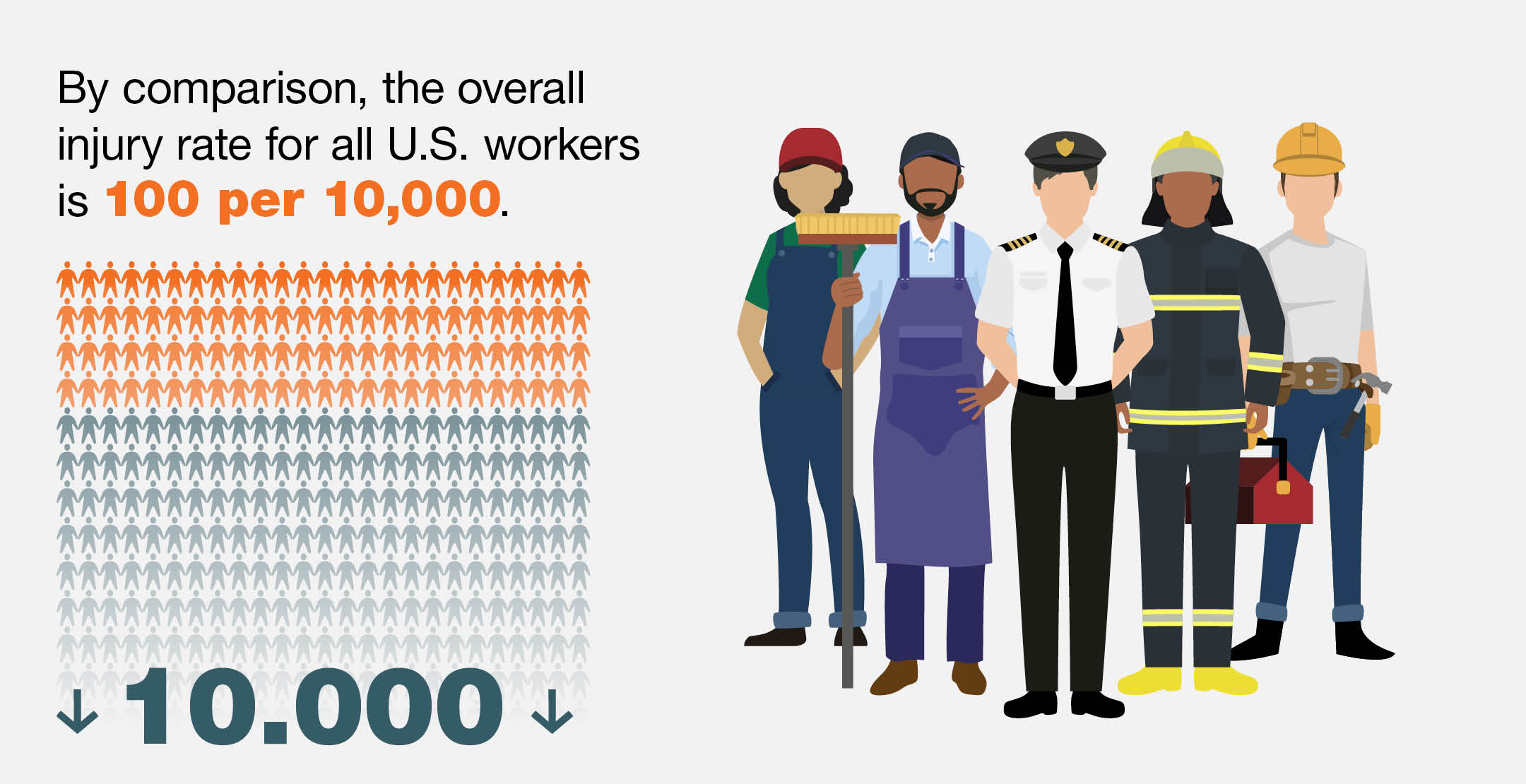
In fact, occupational injury rates for direct care workers are among the highest in the country. According to a report from the New York-based nonprofit PHI, the injury rate for nursing assistants in 2016 was 337 per 10,000 workers. Personal care aides had an injury rate of 144 per 10,000, while for home health aides it was 116. By comparison, the overall injury rate for all U.S. workers was 100 per 10,000.

What makes direct care so dangerous? The answer lies in the nature of the work itself. Assisting patients and residents that are elderly, disabled or otherwise limited in mobility puts a lot of strain on care workers. The leading cause of injury among direct care workers is overexertion, most commonly caused by lifting or repositioning clients.
An article published in the December 2020 issue of the Journal of Occupational and Environmental Medicine found that musculoskeletal injuries that occur during patient handling and mobility (PH&M) tasks are one of the biggest contributors to both employee injuries and workers’ compensation claims.
Taking safety from the bedroom to the bathroom
For caregivers, the bathroom is a common location for workplace injuries as they can experience a lot of physical strain when transferring elderly or a person with physical impairments to and from the toilet, or when helping them bathe. This strain is often intensified by the insufficient physical space and fixed bathroom equipment that doesn’t meet the differing needs of the residents.
However, many facilities can improve worker safety, as well as user independence, by implementing the same safe patient handling and mobility (SPH&M) techniques in the bathroom that are also used in the bedroom.
Boost residents’ confidence, save precious staff time and reduce injuries
Assistive technologies like adjustable beds, slings and lifts are commonplace in the bedrooms of most elderly care and assisted living homes. But not enough facilities use this approach in the bathroom. Customizable solutions would make it easier for staff to assist residents with using the bathroom, it could also minimize, or remove, the need for staff involvement.
Safety solutions like grip bars or shower seats are good, but they’re also the bare minimum for offering support to residents and workers. If the bathrooms were to be equipped with supports arms that are fully adjustable, both vertically and horizontally, and sinks that are height adjustable with a touch of a button, it could limit the amount of help the resident needs in the bathroom. This will improve the caregiver safety while also increasing the independence and dignity of the residents.
How can flexible bathrooms improve your facility?
Facilities can’t afford worker injuries
Reducing workplace injuries is particularly important in light of the care industry’s worker shortage. A sector that has long struggled with recruiting enough workers for what is often low-paying and physically demanding work has been hit hard by both immigration policies and, more recently, the COVID-19 pandemic.
In a November 2021 report, the American Health Care Association and National Center for Assisted Living (AHCA/NCAL), which represent around 14,000 nursing homes and assisted living communities across the United States, said that 221,000 workers have left the industry since the start of the pandemic. That’s a 14 percent overall workforce reduction.


“As many caregivers are getting burned out by the pandemic, workers are leaving the field for jobs in other health-care settings or other industries altogether,” Mark Parkinson, the president and CEO of AHCA/NCAL, said when the report was released.
When a worker is injured while helping a client, it can set off a vicious circle. When the injured worker takes time off to recover, residents miss out on receiving care from someone they’ve come to trust. The worker shortage means that facilities have a difficult time finding a temporary replacement, which often results in the remaining staff members having to shoulder the extra burden. This increases the risk that they will be injured or feel so overworked that they quit their jobs, repeating and accelerating what PHI called “a cycle of unsafe conditions, injuries, and disruptions in care.”


The JOEM article found that an effective way to break that cycle is to invest in SPH&M equipment and train staff on how to utilize it to ease their physical burden. There is also a clear financial incentive for facilities. The article cited one study that concluded that an effective SPH&M program can lead to an average annual net savings of $143 per bed and $165 per full-time equivalent (FTE), while other cited studies found that implementing SPH&M programs reduced patient handling claims in 80 percent of nursing homes and reduced workers’ compensation costs by the same amount.
Similarly, the PHI report concluded that investing in appropriate equipment will result in “cost-savings [that] will likely outweigh the initial investment”.
When considering the data, the advantages of investing in accessible equipment that is safe and flexible are clear. By implementing solutions which can decrease the chance of a workplace injury, facilities are also increasing their residents’ quality of life.
Related articles
You can find more guidance, information and inspiration in the articles listed below.














